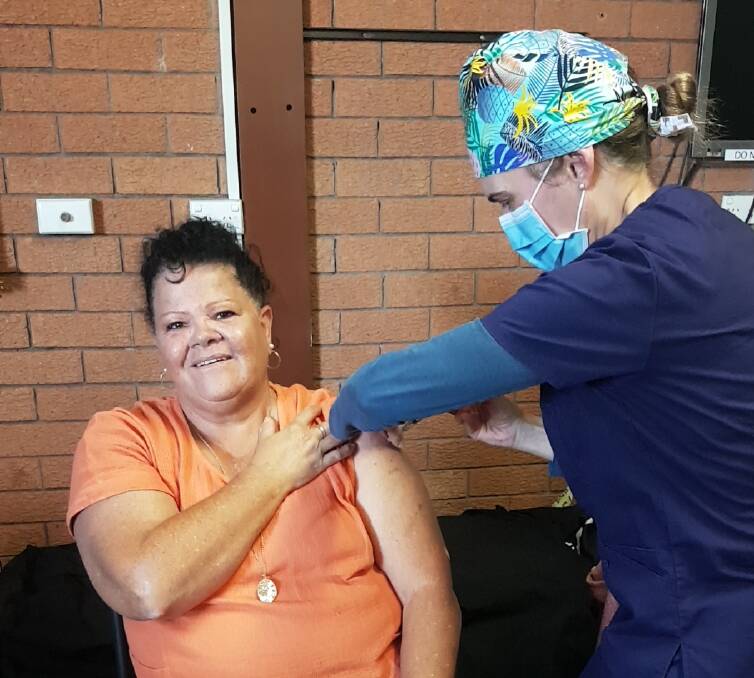
Armajun Health Services has been fighting vaccine hesitancy within Aboriginal communities across the Northern Tablelands for months, but with recent eligibility changes, and an increase in Pfizer supply, that may change - now they are getting the nurses they need to do the job.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
Debbie McCowen is the chief executive officer for Armajun Health Service, which offers primary health care services to Armidale, Inverell, Tingha, Ashford, Glen Innes, and Tenterfield Aboriginal communities.
Ms McCowen said there had been a very slow uptake of vaccination across those communities since the health service started with AstraZeneca, but since they had access to Pfizer, things had improved, particularly in the last few weeks.
"I can't see the hesitancy towards AstraZeneca moving a great deal with our clientele group because they are just firmly opposed to it - and they're scared," she said.
"Every Aboriginal person over the age of 12 years is eligible for the Pfizer vaccine. So if people are willing to have the AstraZeneca, they are being given it, and if they are not, they are being given Pfizer."
Read also:
That hasn't always been the case, Ms McCowen said, but the rules have changed with the recent outbreak of COVID-19 in the Western NSW local health district.
"It's just about getting people vaccinated; it's not about getting hung up with which vaccination," she said.
Ms McCowen said Armajun Health had been getting Pfizer for some time, but they have had an issue with staffing and recently approached Hunter New England Health (HNEH) to give them nurse immunisers to increase the number of clinics and vaccinations they can administer.
"At the moment, we're struggling because our doctors have to do it, and we just can't pump out the numbers that we need," Ms McCowen said.
"We have clinics in Inverell, Glen Innes, and Armidale, and if we get additional support from HNEH, we may be able to do additional clinics in Walcha, Uralla, Guyra, and Tenterfield, but at the moment, we physically can't do it.
"The Commonwealth has said it will double the number of vaccines we have access to so we don't have an issue with supply, but we do have an issue with actually having the capacity to do it."

Dr Kate Martin works for Armajun Health in Armidale and is passionate about the need for Aboriginal people to be vaccinated.
"Vaccination is incredibly important given the vulnerability of the Aboriginal population mainly because of the burden of chronic disease within the Aboriginal community," she said.
"If COVID-19 gets into and spreads through an unvaccinated Aboriginal population, the results are going to be devastating - it will be a national tragedy."
The attitude of the Aboriginal community towards the vaccination is slowly changing, Dr Martin said, but she is furious with the way AstraZeneca was initially portrayed in Australian media.
"I started the clinic with AstraZeneca when we first got it, and there was quite a bit of hesitancy because of the terrible way it has been reported on and people misunderstanding what the risks are," she said.
"AstraZeneca does not increase the risk of regular blood clots, deep vein thrombosis, and strokes. The one-in-a-million side effect of TTS is a different thing that is very rare, very easy to test for, and very easy to treat. "
Anti-vaxxers don't come into the clinics to ask questions, Dr Martin said, and the people that do are open to vaccination, curious, and very receptive.
"They want to hear from an expert what the risks are to them and their families," she said.
"Any hesitancy people have is completely normal and understandable. And after a chat with their doctor, they usually go ahead. A lot of the elders are doing it to set an example for their community which is fabulous."
Now the health service is offering Pfizer, Sharleen Dodd ( the practice manager for the entire Armajun Health Service area) is hopeful the vaccination uptake will increase. Clinics have been running since April, and hundreds of vaccines have already been administered across the region. And there is a need to vaccinate young people 12 and over, Ms Dodd says.
"That needs to be the way in rural areas because we are five hours from a major centre like Newcastle, and we have remote communities dotted in-between our clinics with a high population of people who are very vulnerable and a young demographic," she said.
"Since Pfizer came on board at our clinics, we've seen a big change in attitude.
"What I'm hearing from our Aboriginal and Torres Strait Islander communities is that now that we have Pfizer, their confidence has grown in the vaccine, and people feel safer about making that decision to have a vaccine.
"We're having people coming in wanting to talk to us about the vaccine, we have had many, many phone calls, and we have a waiting list of people wanting the vaccine."
This week Ms Dodd will be given additional workforce by Hunter New England Health, and she says it can't come soon enough. Registered nurse vaccinators have been promised for the Inverell, Armidale, and Glen Innes clinics, and she is in the process of coordinating that effort.
"It's been a lot of work for all the clinic staff up until now, and the good news is that Hunter New England Health has answered the call for additional support to administer the vaccinations and is going to put qualified people in our clinics" she said.
"That's going to make a huge difference and double our vaccination rates."
In Armidale last week, there was a total of 48 vaccines delivered. Inverell had about the same amount, and Glen Innes quite a bit less. There is currently no Tenterfield vaccination clinic, and Armajun Health Service is encouraging that local Aboriginal community to contact their local doctor.
"We could do more, but it is the resource constraints of not having people on the ground to assist because you've still got a clinic to run with people with other conditions and illnesses that need to be seen and require a health care focus," Ms Dodd said.
"With the extra nurses, we'll be looking at administering about 96 jabs a day in Armidale and Inverell.
"In Glen Innes, it's been a bit slower, but it is a smaller community as well. Vaccine clinics are scheduled for two days this week and next week.
"We are still planning Tenterfield, and there are a number of things we are looking at."
HNEH is also bringing along an Aboriginal health worker to the Inverell clinic to assist clients in completing paperwork and explain the information available to them.
Lynette Lackey is a Kunja Baarkinji woman who moved to Inverell 37 years ago from the Darling River area to work in the Department of Community Services. While she doesn't know anyone who has tested positive, she is aware of extended family members in Dubbo and Bourke who are currently in isolation waiting for their test results because they were close contacts of COVID-19 cases.
"I think we've seen an increase in the uptake of vaccination locally because of what we've seen out west and the impact it is having on those Aboriginal communities," Ms Lackay said.
"It's a concern here on the Northern Tablelands because you've got extended families across the region, and they tend to travel to see family."
Ms Lackay has been fully vaccinated for months, and so is most of her family with either AstraZeneca or Pfizer - all with no side effects at all.
"Within our own community and family, we have people with chronic disease, and it's of major concern to our people," she said.
"The reason I did it was mainly because I was concerned about getting Covid, and I was also worried about my family and grandkids.
"When you've got chronic disease in your family, it is even more important because you know what the impact could be - particularly if someone has asthma or heart disease, and I'd hate to give it to someone I knew that is that situation."
Social media is harming the Aboriginal community's confidence in the vaccine, according to Ms Lackay, and the lockdown is taking its toll on morale.
"I think the lockdown is affecting everyone's mental health but especially the Aboriginal population because we like to visit family, and we move around a lot," she said.
"What I'm hearing back from community and others is that they don't believe there has been enough research into the vaccine. Our people don't want to rush into it, and they want to be safe. Recently, there has been a big uptake in people getting the vaccine, but we still have a long way to go.
"If our people are concerned about their vaccination, they need to speak to their doctor to get a better understanding. Then, they can choose the vaccination they want."
Our journalists work hard to provide local, up-to-date news to the community. This is how you can access our trusted content:
- Bookmark armidaleexpress.com.au
- Make sure you are signed up for our breaking and regular headlines newsletters here
- Follow us on Twitter: @ArmidaleExpress
- Follow us on Instagram @armidale.express
- Follow us on Google News


